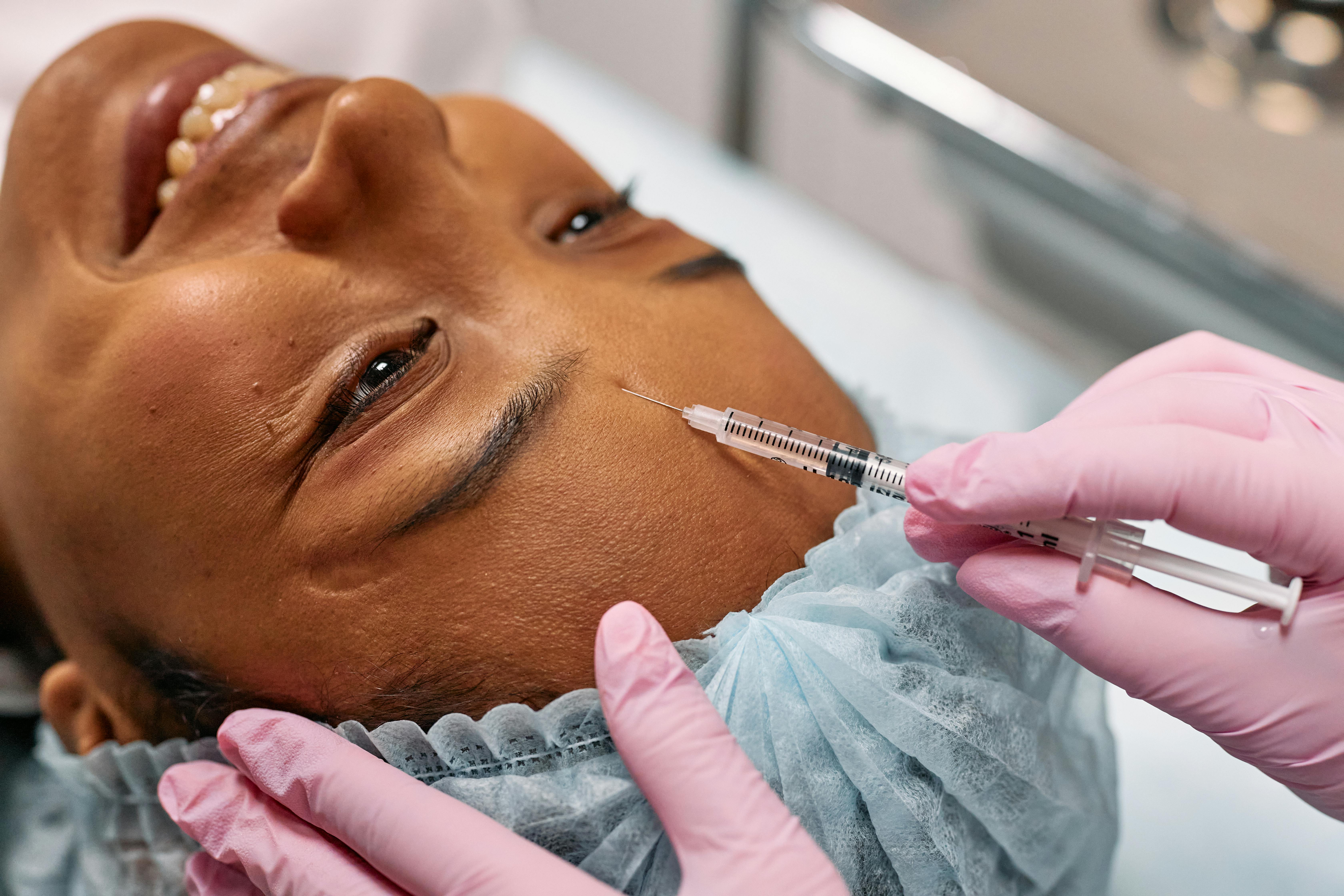
A Look at Today’s Erectile Dysfunction Clinical Trials
Erectile dysfunction clinical trials explore new therapies, medications, and treatment approaches. Understanding the current landscape provides educational insight into research processes, participant roles, and study goals without implying personal eligibility, guaranteed results, or promoting specific trials.
Advances in erectile dysfunction research increasingly come from well-run clinical trials that test whether new treatments are safe, effective, and practical for real patients. In the United States, these studies follow strict ethical and regulatory standards, aiming to answer focused questions and translate results into care that helps more people. Understanding how trials work can make headlines and outcomes easier to interpret and can clarify what participation may entail if you are considering enrolling in your area.
This article is for informational purposes only and should not be considered medical advice. Please consult a qualified healthcare professional for personalized guidance and treatment.
Current erectile dysfunction clinical trials
Across the country, researchers are evaluating a range of approaches. Some studies explore refinements to established therapies such as oral phosphodiesterase type 5 inhibitors, injections, and vacuum devices. Others examine novel pathways that may support erectile function, including nitric oxide signaling modulators, tissue engineering concepts, and neuromodulation. There is ongoing interest in low-intensity shockwave approaches and carefully controlled regenerative strategies, which remain under investigation to clarify who may benefit and under what protocols.
Trial populations are diverse because ED can stem from different causes, such as diabetes, cardiovascular disease, pelvic surgery, neurological conditions, or medication side effects. Inclusion and exclusion criteria screen for safety and scientific clarity. For example, one study might focus on men after prostate surgery, while another targets metabolic risk. Most US trials are registered on ClinicalTrials.gov, where status, eligibility, and locations are listed to help potential participants and clinicians find options in their area.
How ED trials test new treatments
Trial design begins with a clear hypothesis and ends with predefined outcomes. Early phase studies primarily assess safety and dosing, while later phases evaluate effectiveness compared with placebo or current care. Randomization reduces bias by assigning participants to study arms by chance, and blinding helps ensure that expectations do not influence results. Independent monitoring boards routinely review safety data to protect participants while research is ongoing.
Common measures include patient-reported tools such as the International Index of Erectile Function erectile function domain and Sexual Encounter Profile diaries. Objective assessments may include penile Doppler ultrasound to evaluate blood flow and standardized measures of adverse events. Follow-up periods vary by intervention, but researchers often include both short-term and longer-term checkpoints to observe durability of benefit and to watch for delayed effects, which is especially important with device-based or regenerative approaches.
How trials help improve treatment options
Well-conducted studies add clarity to which treatments work, how well they work, and in whom they work best. Results inform clinical guidelines that clinicians use when discussing choices with patients. Trials can show whether a therapy improves erections sufficient for intercourse, whether side effects are acceptable, and how treatments compare in subgroups such as men with diabetes or those recovering from cancer therapy. This evidence helps tailor care so that plans better match individual needs and health histories.
Trials also highlight practical considerations that matter in everyday life, such as ease of use, adherence, and satisfaction for patients and partners. Research can uncover signals that prompt further investigation or identify populations who may need alternative strategies. Diverse enrollment is crucial, because broader participation helps ensure findings apply across ages, ethnicities, and health backgrounds in the United States. Post-approval studies and pragmatic trials then extend insights into real-world clinics to refine how therapies are used.
Current erectile dysfunction clinical trials
For individuals thinking about participation, coordinators share detailed information during informed consent, including potential risks, potential benefits, visit schedules, and responsibilities. Many studies include questionnaires and periodic exams. Some collect blood tests or imaging to track how a treatment works. Participation is voluntary, and you can withdraw at any time. If a trial is not suitable, research teams can often suggest other studies or refer to clinical care pathways.
Because ED can be linked to broader health, trials frequently assess related factors such as cardiovascular risk, sleep quality, or mental health. Integrating these elements helps researchers understand how a therapy fits into overall wellbeing. As evidence accumulates across multiple trials, patterns emerge that can refine dosing, identify predictors of response, and illuminate long-term safety. This cumulative process is how experimental ideas progress toward becoming routine options in clinics.
How ED trials test new treatments
Safety oversight in the United States includes institutional review boards that approve protocols and monitor participant protections. Data safety monitoring boards may pause or stop a study if concerns arise. Transparent reporting ensures that results, positive or negative, inform the field. When trials demonstrate meaningful benefit with acceptable risk, regulators consider whether a therapy should move to broader use, often alongside guidance on training, follow-up, and risk mitigation.
How trials help improve treatment options
Ultimately, clinical trials help transform uncertainty into actionable knowledge. Even when a particular therapy does not outperform standard care, the findings still advance the field by clarifying boundaries and guiding future research questions. Over time, this evidence base supports more personalized approaches, where treatment choices align with the cause of ED, patient preferences, and other health priorities. Better data lead to better conversations and, potentially, better outcomes.
Sources are not included here because no citation links were provided.